What are Some Common Types of Pelvic Floor Dysfunction?
Pelvic Floor Dysfunction (PFD) is defined by the International Pelvic Pain Society as a condition when the pelvic floor muscles do contract, relax, or work together. The pelvic floor is made up of bones, muscles, fascia, and ligaments and functions as a hammock to support the pelvic organs including the uterus, bladder, and rectum. If the muscles become overactive, strained or uncoordinated, they may cause pain in the pelvis. This pain may lead the muscles to not contract, relax, or work together.
What are the muscles of the pelvic floor?
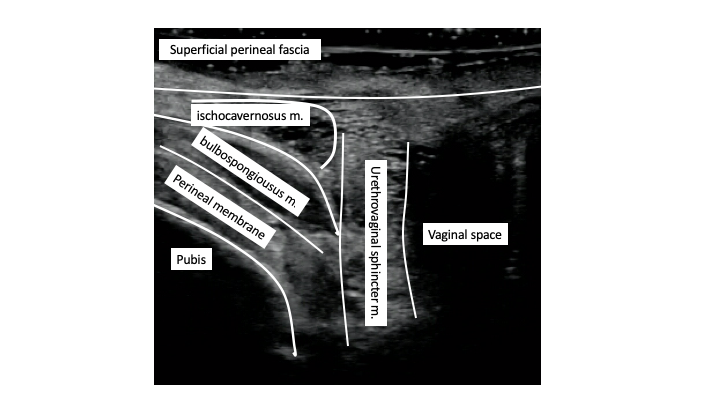
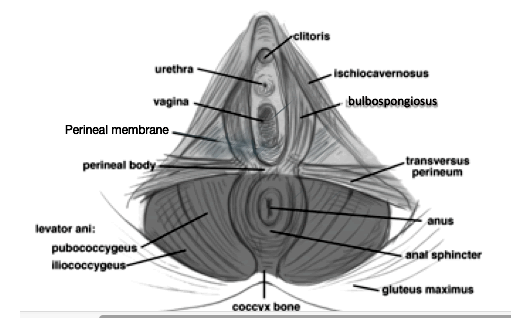
The anterior aspect of the pelvic floor is not well characterized. The entire posterior pelvic floor is referred to collectively referred to as the levator ani, it includes the pubococcygeus, puborectalis, and iliococcygeus. The anterior pelvic floor surrounding the vaginal opening include the bulbospongiosus, ischiocavernosus, transverse perineal muscle, the anterior attachments of the pubococcygeus, perineal membrane, and superficial perineal fascia.
Reference:
Kruger JA, Murphy BA, Heap SW. Alterations in levator ani morphology in elite nulliparous athletes: a pilot study. Aust. N. Z. J. Obstet. Gynaecol. 2005; 45:42-7.
Who gets PFD?
PFD is common. Approximately 1 in 4 women have at least one symptom including pain, urinary incontinence, fecal incontinence, or organ prolapse. There is an increase in prevalence based on age.
Pelvic floor pain and dysfunction affects about 15%-73% of all female athletes with the highest prevalence in gymnasts and acrobatics. The prevalence among dancers is uncertain. Anecdotally, the prevalence among dancers is high.
References:
Nygaard I, Barber MD, Burgio KL, et al. Prevalence of symptomatic pelvic floor disorders in U.S. women. JAMA. 2008; 300:1311-6.
Anderson K, Strickland SM, Warren R. Hip and groin injuries in athletes. Am J Sports Med. 2001;29(4):521–33.
Nygaard IE, Thompson FL, Svengalis SL, et al. Urinary incontinence in elite nulliparous athletes. Obstet. Gynecol. 1994; 84:183-7.
What are the types of pelvic floor dysfunction?
PFD is broadly categorized into 2 types: hypotonic PFD and hypertonic PFD.
Hypotonic PFD is more common, presenting with urinary incontinence, fecal incontinence, or pelvic organ prolapse.
The less common of the two types is hypertonic PFD> Hypertonic PFD symptoms include impaired ability to evacuate urine or stool, sexual dysfunction, and pelvic pain. In this disorder, muscles of the pelvic floor remain in a contracted state causing increased pressure and pain. The pain is persistent and typically worsens throughout the day and with daily activities, such as walking, physical activity, and passing stool. This is anecdotally seen more commonly in gymnasts, dancers, and high-stress professions.
References:
Louis-Charles K, Biggie K, Wolfinbarger A, Wilcox B, Kienstra CM. Pelvic Floor Dysfunction in the Female Athlete. Curr Sports Med Rep. 2019 Feb;18(2):49-52.
Faubion SS, Shuster LT, Bharucha AE. Recognition and management of nonrelaxing pelvic floor dysfunction. Mayo Clin. Proc. 2012; 87:187-93.
Butrick CW. Pathophysiology of pelvic floor hypertonic disorders. Obstet. Gynecol. Clin. N. Am. 2009; 36:699-705.
How is PFD treated?
Soft tissue mobilization of fascial adhesions like Thiele massage can address pelvic pain symptoms, as well as bladder and bowel dysfunction. Movement rehabilitation including lumbopelvic stabilization and core strengthening are critical in resolution of symptoms.
References:
Weiss JM. Pelvic floor myofascial trigger points: manual therapy for interstitial cystitis and the urgency-frequency syndrome. J. Urol. 2001; 166:2226-31.
Pastore EA, Katzman WB. Recognizing myofascial pelvic pain in the female patient with chronic pelvic pain. J. Obstet. Gynecol. Neonatal. Nurs. 2012; 41:680-91.
Montenegro ML, Vasconcelos EC, Candido Dos Reis FJ, et al. Physical therapy in the management of women with chronic pelvic pain. Int. J. Clin. Pract. 2008; 62:263-9. S

